
Nutrition After Colon Surgery . The stomach connects to the small intestine which transitions to become the colon, part of the large intestine. Finally, the large intestine terminates as the rectum. Food and liquid pass through these structures in the process of digestion as nutrients are removed and stool is formed. The segments of the GI system perfom specific, but sometimes overlapping, functions, as explained in detail in . Most nutrient absorption, likewise, occurs in the small intestine. 
Before Surgery for Colon Resection. Before your surgery, you may be asked to follow a special diet to help reduce your discomfort, and should drink plenty of water.The colon also absorbs additional nutrients and electrolytes with the help of the beneficial bacteria that populate the organ. The waste enters the colon in liquid form and is processed into semi- solid form as the colon performs its main function of reabsorbing water into the body. Surgery. Photo Credit NA/Photos. Getty Images. Indications for partial colon resection include limited colon cancers and other pathology that affects only part of the colon. Diverticulitis - - a weakened outpouching of the colon wall - - sometimes requires partial colon removal as well. After partial colon resection, the ends of the colon on either side of the removed segment are sewn or stapled back together. Removal of the entire colon, a total colectomy, cures ulcerative colitis and familial polyposis, a genetic condition in which precancerous polyps develop throughout the large intestine. After a total colectomy, the end of the small intestine- -the ileum- -can be sewn back to the rectum. The other option uses an ileostomy, either temporarily or permanently. Most of what I found were what to expect after. Since none of the digestive-related forums really fit my situation, I'm posting this in the "irritable bowel" forum (for lack. Surgery Overview. Resection is another name for any operation that removes tissue or part of an organ. Bowel resection, also called partial colectomy, removes a. The large intestine, also known as the large bowel or colon, is the last part of the gastrointestinal tract and of the digestive system in vertebrates. 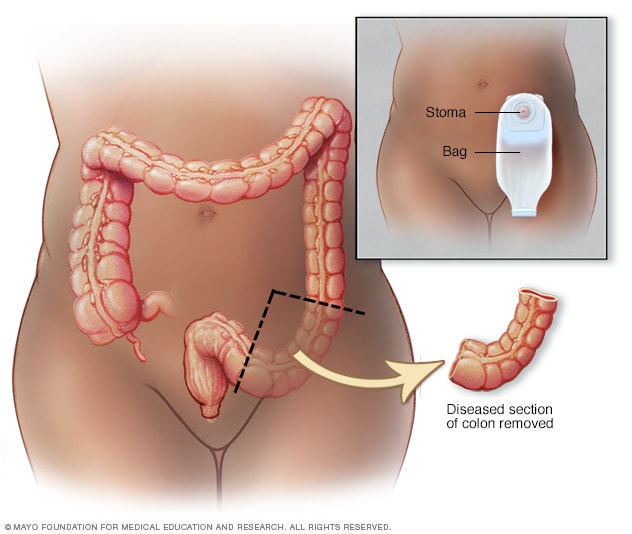
With an ileostomy, the end of the small intestine is connected to the outside of the body through an opening created in the abdominal wall and waste is collected in special bags that attach to this opening. Glass of water. Photo Credit Jupiterimages/Photos. Getty Images. Removing any part, or all, of the five- foot long colon leads to changes in the process of stool formation. Nutrition, both in the immediate post- operative period and the long term requires special consideration. In the days after surgery, a liquid diet ensures that the suture or staple line begins to heal properly without disruption from irritating food substances. 
Usually within a few days, introduction of soft foods begins. If this progresses as expected, significant nutritional deficits rarely occur, especially with partial resection. If advancing the diet proves difficult, nutrition temporarily comes from intravenous solutions that contain essential nutrients such as proteins and fats, explains the American Society of Colon and Rectal Surgeons on its website. Stool frequency after surgery sometimes tops 2. Because electrolytes and water are eliminated in this liquid stool, disturbances of electrolyte balance and dehydration present the most significant risks in the days after colon surgery. Sodium, potassium, calcium and magnesium levels warrant daily testing in the initial post- operative period. Avoiding dehydration presents the biggest challenge in the immediate days after surgery. Intravenous fluids replace losses until oral intake of water catches up. Soup and liquid foods break down easily. Photo Credit Jupiterimages/Goodshoot/Getty Images. Over time, the body adapts to the loss of part or all of the colon. The small intestine takes over the function of absorbing water and dehydration becomes less of an issue. Electrolyte salvage also becomes more efficient in the small intestine. With total colectomy, nutritional risks persist for weeks or months. Any abdominal surgery leaves the risk of adhesions and obstructions for a lifetime, states the Nov. Obstruction of the intestine, sometimes a medical emergency, becomes more likely with adhesions. Many doctors and patients find that this has nutritional implications. Foods, such as raw vegetables, mushrooms, nuts and seeds that digest and break down less easily, cause obstructions and sometimes require elimination from the diet.   
After colon surgery, supplements and vitamins can help to make up these deficits. Nutritionist. Photo Credit Creatas/Creatas/Getty Images. The main objectives of avoiding dehydration and maintaining a balanced diet challenge patients and surgeons. Referral to a nutritionist or dietitian prior to elective surgery allows patients to plan ahead for expected dietary and nutritional changes. Especially after total colectomy, reintroduction of foods occurs very slowly in some cases, and working with the nutritionist provides the best method of assessing and supplementing any deficits. Following the recommendations of the doctors and nutrition experts ensures the smoothest recovery possible. New Guidelines on Acute Diverticulitis: How Will They Change Clinical Practice? Ostomy Overview. An ostomy is a surgical procedure performed when normal bowel or bladder function is lost due to birth defects, disease, treatment for disease, or. References for "Colon Blockage" (1) J.J. Tuech, M.D., P. Pessaux, and J.P. Arnaud, M.D. Learn about colostomy surgery, colostomy care, colostomy questions, and information about colostomy recovery. Find out how one patient learned to live with a. Colonic Diverticular Disease. Colonic diverticulosis is among the most common diseases in developed Western countries. In the United States, diverticulosis occurs in approximately one third of the population older than age 4. Definition and causes. A diverticulum is a saclike protrusion in the colonic wall that develops as a result of herniation of the mucosa and submucosa through points of weakness in the muscular wall of the colon. The colonic diverticulum is a false or pulsion diverticulum- that is, it does not contain all layers of the colonic wall. Diverticulosis indicates the presence of multiple diverticula and generally implies an absence of symptoms (Fig. Diverticular disease implies any clinical state caused by diverticula, including hemorrhage, inflammation, or their complications. Diverticulitis describes the presence of an inflammatory process associated with diverticula. Its pathogenesis is attributed to genetic and environmental factors (Box 1). Box 1: Factors Involved in the Pathogenesis of Colonic Diverticula. Genetic factors. Environmental factors. Low- fiber diet. Obesity. Decreased physical activity. Corticosteroids. NSAIDs. Alcohol. Caffeine intake. Cigarette smoking. Polycystic kidney disease. Epidemiologic factors. Age. Geography. Life style. Ethnicity. Back to Top. Prevalence. The actual prevalence of diverticulosis is difficult to measure because most individuals are asymptomatic. Comparisons of the earliest and most recent autopsies and barium enema studies have indicated that the worldwide prevalence is increasing over time (Box 2). Box 2: Prevalence of Diverticulosis. Studies so far include barium examinations and necropsy series. These may be misleading for determining the actual prevalence rate, however, mainly because barium studies may overestimate the prevalence of diverticulosis in people who have been referred for gastrointestinal (GI) symptoms, and necropsy series may either overestimate the frequency of diverticula in older age groups or miss the presence of small diverticula in younger populations. Whether these findings are the results of increased numbers of older individuals in the population, increased screening, or an actual increase in prevalence is unknown. Younger patients presenting earlier than age 4. Back to Top. Pathophysiology. Colonic diverticulosis in general is an acquired disease, developing as mucosal and submucosal herniations through the circular muscle layer at vulnerable weak points of the colonic wall. Diverticula are covered only by serosa, and tend to develop at four well- defined points around the circumference of the colon, where the vasa recta penetrate the muscular layer. These vessels enter the colonic wall on either side of the mesenteric teniae and on the mesenteric border of the two antimesenteric teniae. Diverticula do not develop in the rectum, presumably because of the coalescence of the teniae with the longitudinal muscle layer that marks the junction between the sigmoid colon and the rectum. In the colon, the presence of anatomic and physiologic changes contributes to the development of diverticula (Box 3). Mycosis, a set of findings consisting of the thickening of the muscular layer, shortening of the teniae, and luminal narrowing, is found in most patients with sigmoid diverticula. Box 3: Physiologic and Anatomic Colonic Changes in Diverticula Formation. Mycosis. Changes in mechanical features of colonic wall. Changes in structural components of colonic wall. Elevated intraluminal pressure. Segmentation. The mechanical features of the colonic wall change with increasing age. Combined barostat- manometry studies of the entire colon have demonstrated that compliance is lowest in the sigmoid and descending colon and greatest in the transverse and ascending colon. This difference in mechanical properties between the right and left sides might partly account for the left- sided predominance of diverticulosis. Structural components of the extracellular matrix of the colonic wall, including collagen, elastin, and proteoglycans, are likely to be important in maintaining the strength and integrity of the colonic wall. Changes in these components of the bowel wall, such as damage and breakdown of mature collagen, and consequently its immature synthesis can lead to a change in bowel consistency. These changes may be related to a genetic predisposition such as that seen in Ehlers- Danlos and Marfan's syndromes, which may be responsible for the occurrence of diverticula at an early age, or to the natural course of the aging process itself. In one study, it has been reported that collagen fibrils in the left colon are smaller and more tightly packed than those in the right colon with increasing age, and that this difference is accentuated in diverticular disease. The thickening of longitudinal and circular muscles in diverticular disease is neither hyperplastic nor hypertropic, but appears to be related to a contractile state. An increase in the number of elastic fibers has been observed only in the longitudinal muscle. It has been suggested that this process is responsible for longitudinal contraction, with subsequent thickening of both muscle layers. All these changes, along with elastin deposition in the teniae coli, lead to an irreversible state of contracture, with substantial bowel shortening, which may result in decreased resistance of the colon wall to persistent intraluminal pressure. In addition to other predisposing factors, diverticula are believed to develop as a result of elevated intraluminal pressure generated by tonic and rhythmic contractions, resulting in segmentation. If contractions occur relatively close to each other and form an enclosed space, pressure within that intervening segment of colon may exceed 9. Hg. However, segmentation on its own separates the colonic lumen into a series of chambers, with each having a different amount of pressure that is closely related to the chamber's diameter. These isolated increases of intraluminal pressure are believed to predispose to herniation through the previously mentioned weak points of the colon. The fiber content of the diet plays a large role in the pathogenesis of diverticular disease. Fiber has been found to be protective. Most fiber in the human diet is of plant origin and this type of fiber binds water and salt in the colon, leading to bulkier and more voluminous stools. Therefore, fiber decreases the frequency of contractions and prevents an exaggerated form of segmentation. In addition, dietary fiber influences the content of colonic bacterial flora, forms the main substrate for bacterial carbohydrate fermentation, and produces energy- yielding substrates—short- chain fatty acids—for growth and maintenance of colonic cellular function. Consequently, a fiber- deficient diet increases the chances of intense, more frequent segmentation, thus predisposing to herniation of mucosa by allowing isolated increases of intraluminal pressure. After the development of colonic diverticula, a spectrum of inflammatory changes or bleeding caused by the traumatic injury to penetrating vessels may occur. Changes within these vessel walls, such as eccentric intimal thickening and thinning of the media of the vessel facing the bowel lumen, result in segmental weakness of these vessels and render them vulnerable to injury and bleeding. The term diverticulitis represents a spectrum of inflammatory changes that ranges from localized subclinical inflammation to generalized peritonitis, with free perforation (Fig. In turn, this leads to hyperplasia of the lymphoid tissue within the mucosa at the base of the diverticulum, one of the earliest signs of diverticulitis. Inflammation usually begins at the apex of the diverticulum and seldom involves the neck or mucosa proximal to the neck. However, there is active inflammation of the pericolic and mesenteric fat, with peridiverticular abscess formation. These peridiverticular abscesses often involve areas of subserosa and are closely related to the outer aspect of the muscularis propria; they can spread circumferentially and longitudinally and may be responsible for the pathologic picture of diverticular colitis. Longitudinal tracking, especially, may result in fissuring, along with the lymphoid aggregates, which resembles the distinctive feature of colonic colitis in Crohn's disease. This may cause misinterpretation of the pathologic study of the specimen. Therefore, the differential diagnosis of these two conditions in terms of pathologic interpretation of the resected specimen is important. Persistent localized inflammation after diverticular rupture results in a phlegmon, a thickened, firm segment of bowel wall, which ultimately may manifest as acute or subacute large bowel obstruction. If left untreated or treated inadequately, it may result in extensive fibrosis around the affected segment of the colon, giving it a mass appearance indistinguishable macroscopically from that of a neoplasm. Another pathologic entity that may be encountered during progression of the disease, with recurrent attacks of diverticulitis, is the formation of a localized abscess with chronic inflammation and involvement of other neighboring luminal organs, such as the bladder, small and large bowel loops, uterus, and vagina. Fistulae may develop within this contained area, between involved segment(s) of colon and these organs. Fistulae occur in 2. Back to Top. Signs and symptoms. Most people with uncomplicated colonic diverticulosis are asymptomatic. A small fraction of these patients may have troublesome symptoms, such as colicky abdominal pain, bloating, flatulence, or altered bowel habit. The symptoms characteristically disappear after defecation or passage of flatus. On clinical examination, they may have tenderness in the left iliac fossa with no signs or symptoms of peritonitis or systemic illness, and all laboratory values may be within normal limits.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
